Perineal Nerve
Introduction
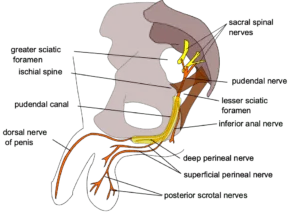
The perineal nerve is a big terminal branch of the pudendal nerve that normally begins during its passage through the pudendal canal or shortly after it exits the canal. The pudendal nerve travels to the perineum before splitting into two terminal branches: the superficial perineal nerve (superficial perineal branch) and the deep perineal nerve.
The perineal nerve is a mixed nerve. Its sensory fibers are supplied by the superficial (sensory branch), while its motor fibers flow through the deep. This nerve’s major function is to send sensory and motor information to the urogenital triangle structures in both sexes.
Structure
The perineal nerve is an extension of the pudendal nerve. It is located underneath the internal pudendal artery. It travels alongside the perineal artery. It goes into the pudendal canal for about 2 or 3 cm. Whilst remaining in the canal, it separates into superficial branches and a deep branch. The superficial branches of the perineal nerve develop into the posterior scrotal nerves in males and the posterior labial nerves in women.
The perineal nerve’s deep branch, commonly known as the “muscular” branch, nourishes the muscles of the perineum. Both are superficial to the dorsal nerve of the penis or the dorsal nerve of clitoris.
Function
Sensory Functions
The perineal nerve provides cutaneous feeling through its two major branches:
The posterior scrotal and labial sensory branches originate from the superficial perineal nerve.
Males produce skin for the perineum and posterior scrotum, whereas females offer skin for the labia minora and majora.
In females, the deep perineal nerve transmits feeling to the vestibule and inferior vagina.
Motor Functions
- Bulbospongiosus
- Ischiocavernosus
- Superficial transverse perineal muscle
- External urethral sphincter
- Levator ani muscle
Course
The perineal nerve is a branch of the pudendal nerve that passes anteriorly through the perineum together with the perineal artery. It usually starts in the last section of the pudendal canal (within the Alcock’s canal) or right as the pudendal nerve exits the canal. The perineal nerve terminates in a bifurcation shortly after leaving the canal.
Branches
The perineal nerve gives off two terminal branches. These branches include:
- The superficial perineal nerve
- The deep perineal nerve
Superficial perineal nerve
In men, the superficial branch innervates the posterior scrotal region, whereas in females, it innervates the labia minora, vaginal vestibule, and the posterior side of the labia majora. It also supplies sensory information to the bulk of the skin covering the urogenital triangle.
Deep perineal nerve
The deep perineal nerve is also referred to as the muscular or motor branch of the perineal nerve. This branch supplies the urogenital triangle muscles (bulbospongiosus, ischiocavernosus, and superficial transverse perineal muscle), the external urethral sphincter, the front sections of the external anal sphincter, and the levator ani. The deep perineal nerve supports micturition and sexual function (i.e., erection and ejaculation).
Furthermore, this branch transmits somatic sensations from all structures in the male and female superficial perineal spaces, including erectile, muscular, and glandular tissues, as well as the lower fifth of the vaginal canal.
Clinical Importance
Perineal nerve injury
Perineal nerve injuries are not particularly prevalent. However, when they do occur, the effects can be devastating. This nerve is most commonly wounded in vehicle or motorbike accidents, falls to the perineum, sexual abuse, or other traumatic injuries. The most prevalent signs of perineal nerve damage are bladder control issues and sexual dysfunction.
FAQs
What are the symptoms of perineal nerve damage?
Other symptoms include:
Increased sensitivity, such as discomfort while putting on pants.
Feeling bloated in your perineum (as if there is an item in your anus).
Feeling an urgent need to pee.
Painful bowel movements.
Painful sex.
Trouble reaching orgasm.
Erectile dysfunction.
What is the perineal nerve of S4?
The perineal branch of S4 is a mixed motor and sensory nerve from the sacral plexus, not to be confused with the perineal branch of the pudendal nerve.
How do you treat perineal nerve damage?
Peroneal Nerve Injury Treatment
Nonsurgical therapies such as orthotics, braces, and foot splints that go inside shoes can provide relief. Physical therapy and gait retraining can help people improve their mobility.
What causes perineal nerve damage?
Causes of PNE
Repetitive mechanical injury (from cycling for long periods) Childbirth. An injury occurred after surgery to the pelvic area. Tumors or lesions in the pelvis.
How do you heal the perineal nerve?
If you have peroneal nerve damage, you may have numbness in the lower leg or foot. Many folks experience a foot drop. Common treatments for peroneal nerve injuries include shoe inserts, physical therapy, and gait training. Nonsurgical therapy can often alleviate or eliminate symptoms.
References
- Wikipedia contributors. (2024b, May 3). Perineal nerve. Wikipedia. https://en.wikipedia.org/wiki/Perineal_nerve
- TeachMeAnatomy. (2024c, June 25). Perineal nerve – course – Supply – TeachMeAnatomy. https://teachmeanatomy.info/encyclopaedia/p/perineal-nerve/
- Perineal nerve. (2023, November 3). Kenhub. https://www.kenhub.com/en/library/anatomy/perineal-nerve