Sciatic Nerve
Introduction
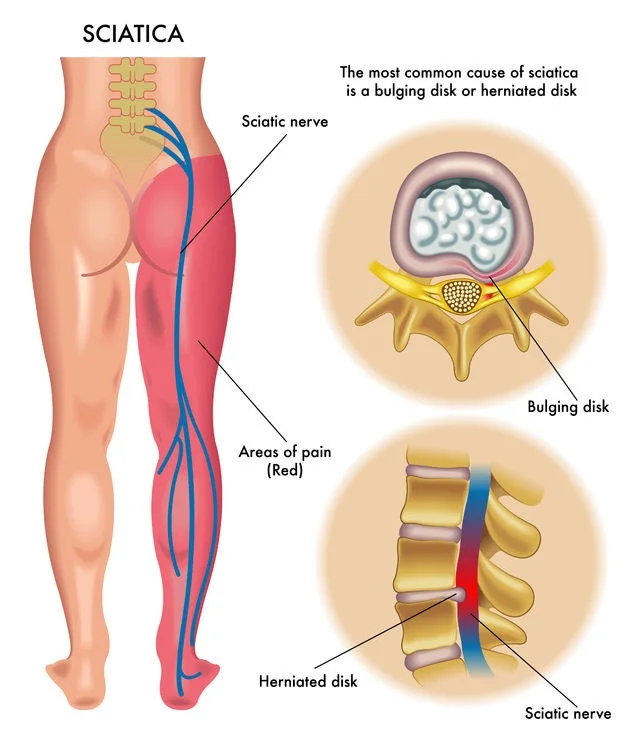
The sciatic nerve is the largest and longest nerve in the human body, originating from the lumbar and sacral spine (L4-S3). It runs through the buttocks and down the back of the leg, supplying motor and sensory function to the lower limbs. Compression or irritation of the sciatic nerve can lead to sciatica, causing pain, numbness, or weakness along its pathway.
The nerve is derived from the ventral rami of spinal nerves L4–S3 and comprises fibres from both the posterior and anterior divisions of the lumbosacral plexus. After leaving the lower vertebrae, the nerve fibres join to create a single nerve. It leaves the pelvis via the larger sciatic foramen behind the piriformis muscle, with the pudendal nerve and vessels, inferior gluteal nerve and vessels, nerve to obturator internus, and posterior femoral cutaneous nerve.
The sciatic nerve then travels along the posterior compartment of the thigh, passing deep to the long head of the biceps femoris muscle, superficial to the adductor magnus and short head of the biceps femoris muscle, and laterally to the semitendinosus and semimembranosus muscles.
Just before reaching the popliteal fossa, it divides into two main branches. The tibial nerve is a branch that continues to descend into the leg and the foot’s posterior compartments. The other branch is the common peroneal nerve, which connects the lateral and anterior compartments of the leg and foot. Before to this separation, the medial component was referred to as the tibial division or the sciatic nerve’s common fibular (peroneal) division.
Structure
The sciatic nerve supplies motor innervation to the posterior compartment of the thigh. This includes the biceps femoris, semimembranosus, semitendinosus, and ischial component of the adductor magnus, which enable knee flexion and hip adduction.
The gastrocnemius, soleus, plantaris, popliteus, flexor hallucis longus, flexor digitorum longus, and tibialis posterior muscles are all innervated by the tibial nerve.
The common fibular (peroneal) nerve innervates the leg and foot’s anterior and lateral compartments. The anterior compartment houses the tibialis anterior, extensor hallucis longus, extensor digitorum longus, and fibularis tertius.
The sciatic nerve also innervates the skin of the foot and lower leg (except the medial leg, which is innervated by the saphenous nerve). The tibial nerve is further divided into medial and lateral plantar nerves, which are responsible for sole feeling. The common fibular (peroneal) nerve is further divided into the superficial fibular (peroneal) nerve and the deep fibular (peroneal) nerve.
The superficial fibular nerve innervates the lateral leg and the dorsum of the foot. The deep fibular nerve transmits feeling between the first and second toes. The medial and lateral sural nerves are made up of collateral branches from the tibial and common fibular nerves, and they supply sensation to the calf and a little lateral area of the foot.
Course
It extends from the ventral rami of the fourth lumbar to the third sacral spinal nerves and is a continuation of the sacral plexus’s upper half.
It exits the pelvis via the greater sciatic foramen, located below the Piriformis muscle, and descends between the greater trochanter of the femur and the ischial tuberosity. It starts deep to the piriformis and goes inferiorly and laterally posterior to the ischium, passing the nerve to the quadratus femoris. It is located underneath the piriformis and extends deep into the Gluteus Maximus. It runs inferiorly through the Obturator Internus, the Gemelli Muscles, and the Quadratus Femoris.
The medial side contains the Posterior Femoral Cutaneous Nerve and the Inferior Gluteal Artery. Descending vertically, it enters the thigh at the lower border of the gluteus maximus and rests on the posterior surface of the Adductor Magnus. Nerves branch out into hamstring muscles. The Biceps Femoris’ long head crosses the nerve obliquely on its superficial appearance. The nerve terminates in the upper side of the popliteal fossa, where it divides into distal nerves (tibial and common peroneal nerve).
Before diverging, the tibial and common peroneal nerves are anatomically distinct and only weakly connected to the sciatic nerve. The tibial nerve originates from the sacral plexus’s anterior divisions, whereas the common fibular nerve is composed of the plexus’s posterior divisions.
On the back of the thigh, draw a line from the ischial tuberosity to the apex of the greater trochanter down to the apex of the popliteal fossa.
Function
Motor Functions
The sciatic nerve travels through the gluteal area but does not innervate any of the muscles there. However, the sciatic nerve directly innervates the muscles in the thigh’s posterior compartment as well as the hamstring component of the adductor magnus.
The sciatic nerve indirectly innervates numerous additional muscles through its two terminal branches:
Tibial nerve – The posterior leg muscles (calf muscles), as well as part of the foot’s intrinsic muscles.
Common fibular nerve –The anterior and lateral leg muscles, as well as the remaining intrinsic foot muscles.
The sciatic nerve innervates the muscles of the posterior thigh, the whole leg, and the foot.
Sensory Functions
The sciatic nerve lacks any direct cutaneous functions. It provides indirect sensory innervation through its terminal branches:
Tibial nerve – provides skin for the posterolateral leg, lateral foot, and sole.
Common fibular nerve – provides skin for the lateral leg and the dorsum of the foot.
Muscle Supply
The sciatic nerve comes from the larger sciatic foramen located under the piriformis. It is divided into two sections: medial (tibial) and lateral (common fibular). Compton-Cruveilhier’s septum divides the two sections. The tibial division innervates the back half of the adductor magnus, the semitendinosus, the semimembranosus, and the long head of the biceps femoris. These hamstring muscles originate in the ischial tuberosity. They are long, stringy muscles that originate from the ham (buttock).
The common fibular nerve supplies the thigh’s short head of the biceps femoris muscle.
The tibial nerve innervates both the superficial and deep posterior compartments of the leg. The superficial posterior compartment contains the triceps surae (medial and lateral heads of the gastrocnemius and soleus), as well as the plantaris and popliteus. The tibial nerve also innervates the plantaris and popliteus. The deep posterior compartment houses the tibialis posterior, flexor digitorum longus, and flexor hallucis.
The common fibular nerve is divided into two parts: the superficial fibular nerve, which innervates the fibularis longus and fibularis brevis in the lateral compartment of the leg, and the deep fibular nerve, which innervates the tibialis anterior, the extensor digitorum longus, the extensor hallucis longus, the extensor hallucis brevis, the extensor digitorum brevis, and the first lumbrical. A key clinical feature is that the deep fibular nerve innervates the area between the large and second toes. The deep fibular nerve provides sensory innervation to this area of the foot exclusively.
The lateral plantar nerve corresponds to the ulnar nerve in the hand. It innervates the adductor hallucis, flexor digiti minimi brevis, lumbricals 2–4, four dorsal interossei, and three palmar interossei.
Branches
Articular branches emerge proximally to nourish the hip joint via its posterior capsule, which can occasionally originate from the sacral plexus.
Muscular branches supply the hamstring muscles and the ischial portion of the adductor magnus.
The tibial and common peroneal nerves are the distal terminal branches.
Embryology
Neurulation begins in the third week following fertilisation. It begins when a layer of cells above the ectoderm thickens, forming the neural plate. The neural plate connects the neural tube and neural crest cells. The neural crest cells will produce neurones in the peripheral nervous system, including the sciatic nerve. Furthermore, neural crest cells give rise to Schwann cells, which are important for peripheral nervous system myelination.
Anatomical Variations
The undivided sciatic nerve typically leaves the larger sciatic foramen, which is inferior to the piriformis, although this is not always true. In the most common anatomic variant, the sciatic nerve separates above the piriformis, with one division exiting via the piriformis and the other below. The present literature describes six anatomical variations.
- Type I: The sciatic nerve exits inferior to the piriformis, undivided. This is the most prevalent type.
- Type II: The sciatic nerve separates above the piriformis, with one section exiting through it and the other inferior to it. The common fibular (peroneal) division runs through the piriformis. This is especially troublesome when the common fibular nerve is located between the two piriformis tendons. In 10% of cases, the sciatic nerve traveled through or above the piriformis.
- Type III: The sciatic nerve separates above the piriformis; one component runs anterior to the piriformis and the other posterior to it.
- Type IV: The sciatic nerve exits via the piriformis, undivided.
- Type V: The sciatic nerve separates above the piriformis, with one section exiting through the piriformis and the other superior to it.
- Type VI: The sciatic nerve splits from the superior portion of the piriformis posteriorly, undivided.
Examination
A neurological examination is critical for determining the status of the sciatic nerve.
Straight leg raise test
The Straight Leg Raise Test (SLR) is a neurodynamic test. Neurodynamic examinations examine the mechanical mobility of neurological tissues, as well as their susceptibility to mechanical stress or compression. These tests, together with relevant history and limited range of motion, are regarded by some as the most crucial physical indicators of disc herniation, regardless of the severity of the injury.
Slump test
The slump test is a nerve tension test for the sciatic nerve. It is a provocative test in which the sciatic nerve is stretched by stretching the spine, hips, and knees. To begin the exam, have the patient sit with hands behind their back to establish a neutral spine. The initial phase involves having the patient slouch forward at the thoracic and lumbar spines. If this posture does not produce pain, have the patient stretch the neck by resting the chin on the chest and extending one knee as far as possible.
If extending the knee creates discomfort, instruct the patient to extend the neck to neutral. If the patient is still unable to extend their knee owing to discomfort, the test is termed positive.
If extending the knee does not create discomfort, have the patient actively dorsiflex the ankle. If dorsiflexion produces discomfort, have the patient slightly flex the knee while remaining dorsiflexed. If the pain is recreated, the test is considered to be positive.
Clinical Importance
Piriformis Syndrome
Piriformis syndrome is caused by a swollen piriformis that compresses the sciatic nerve or one of its divisions (tibial and/or common fibular division). The common fibular division crosses over the piriformis muscle in Beatty and Anson types, as well as Robinson types C and III. This has been proven surgically and by an intraoperative EMG investigation in which stimulation of the sciatic nerve elicited dorsiflexion in the foot. The piriformis muscle was divided using a transgluteal surgical technique, resulting in a cure.
Piriformis syndrome causes hip discomfort that extends down the lower leg. The discomfort worsens whether driving or sitting. Unlike a herniated disc, piriformis syndrome does not cause paralumbar muscular spasm. The prevalence of piriformis syndrome is believed to be around 16%. Piriformis syndrome is thought to be the most prevalent cause of extraspinal sciatica.
Ultrasound guidance of the lidocaine injection can be utilised in an emergency department to treat piriformis syndrome.
In an MRI examination of 254 sciatic nerves in 127 people, the sciatic nerve and piriformis muscle in patients with piriformis syndrome showed higher T2 signal intensity. Splitting of the sciatic nerve was seen in 56/64 compared to 20/190 control patients (P<0.0001). The symptomatic side showed an increase in the sciatic nerve, piriformis size, and T2 signal intensity.
The posterior portion of the piriformis syndrome is very significant when doing hip arthroplasty, sciatic nerve blockade, or image-guided piriformis syndrome injections.
One theory is that damage to the piriformis triggers the production of inflammatory mediators, which cause swelling of the piriformis and compress the sciatic nerve divisions.
Surgical Importance
Sciatica is described as irritation or compression of the sciatic nerve, which produces discomfort in the buttocks and radiates down the leg. The great majority of instances are caused by a spinal condition, such as a herniated or ruptured disc, resulting in L5 or S1 nerve root impingement. Other frequent reasons are spinal stenosis, degenerative disc disease, and spondylolisthesis. Other non-spinal causes of sciatica are less prevalent. These include piriformis syndrome, trauma, surgical problems, gynaecological disorders, and herpes zoster.
Symptoms include mid-buttock discomfort that spreads down the leg, typically unilaterally. Depending on where the sciatic nerve is inflamed, the patient may suffer paresthesias in a dermatomal distribution, such as L5 or S1. Weakness and reflex alterations occur less often. L5 has no reflexes. S1 is the ankle-jerk reflex.
The Lasegue straight leg raising with the patient supine is a test that should always be performed in patients with lower back discomfort. The test is positive if there is ipsilateral discomfort ranging from 10 to 60 degrees. This test is highly sensitive (90%) but lacks specificity. If this test causes discomfort in the contralateral limb, a disc herniation should be suspected and an imaging test ordered. When the precise degree of compression in the spine is unknown, an MRI can be quite beneficial.
MRI can also detect soft tissues (including discopathy), infections, and malignant causes. If a patient with sciatica has urinary retention or dysesthesia around the anus, cauda equina syndrome should be suspected. This disease requires prompt surgical decompression.
The majority of sciatica cases are treated conservatively, which includes a few days of rest, pain medication, and physical therapy. Surgery may be indicated in situations of severe stenosis or nerve irritation.
FAQs
What are the 4 stages of sciatica?
Sciatica has four stages: acute, subacute, chronic, and resolution. Stage One: Acute Sciatica, the most common type of sciatica, develops when a herniated disc or spinal stenosis compresses or irritates the sciatic nerve. Symptoms may include tingling, numbness, and weakness in the lower back or legs.
How do you relieve sciatic nerve pain?
Other self-care treatments that might help include:
Cold packs. Apply a cold compress to the uncomfortable area for up to 20 minutes multiple times each day.
Hot packs. After two to three days, apply heat to the painful regions.
Stretching. Stretching exercises for the lower back might provide some relief.
Medications.
Do I need an MRI for sciatica?
While an MRI can help identify the cause of sciatica, it’s not always necessary and is often considered later in the diagnostic process, especially if conservative treatments haven’t been effective or if there are concerning symptoms.
How to sleep with sciatic pain?
It is more pleasant to sleep on the pain-free side, with the sciatic side on top. To support the spine and pelvis, bend the knees and insert a cushion between them. If there is a space between the waist and the mattress, insert a little cushion. A cushion may be required for arm support as well.
What is the quickest way to stop sciatica?
Ice packs (or even a bag of frozen peas) can help decrease inflammation and feeling in the sciatic area. Apply an ice pack to the aching region for a few minutes until you feel relief. If ice packs do not work for you, a heat pack or hot water bottle may be more effective.
References
- TeachMeAnatomy. (2025a, February 8). The Sciatic Nerve – course – motor – sensory – TeachMeAnatomy. https://teachmeanatomy.info/lower-limb/nerves/sciatic-nerve/
- Sciatic Nerve (2023, November 16).StatPearls.https://www.ncbi.nlm.nih.gov/books/NBK482431/

2 Comments