Effort Thrombosis (Paget-Schroetter Syndrome)
Introduction
Effort thrombosis, also known as Paget-Schroetter Syndrome, is a form of deep vein thrombosis (DVT) that affects the upper extremity, typically occurring in athletes or individuals engaged in repetitive overhead activities. It results from compression and injury to the subclavian vein, leading to clot formation.
Symptoms include swelling, pain, discoloration, and a feeling of heaviness in the affected arm. Early diagnosis and treatment—ranging from anticoagulation to thrombolysis and possible surgical intervention—are crucial to prevent complications such as post-thrombotic syndrome.
Paget-Schroetter syndrome (PSS) is characterized by compression of the subclavian vein at the thoracic outlet and effort-induced thrombosis of the axillary and subclavian veins. The symptoms of thoracic outlet syndrome (TOS), which is the venous form, are linked to compression of the brachial plexus, subclavian vein, or subclavian artery as they pass through the thoracic outlet. This phenomenon was first described in 1875 when Sir James Paget described a patient who had developed spontaneous thrombosis of the subclavian vein. Von Schroetter postulated in 1884 that the disorder resulted from repetitive musculoskeletal action that damaged the vein.
Compression of the thoracic outlet structures as they leave the thoracic cavity is known as thoracic outlet syndrome (TOS). Variations in its presentations can be defined to any of the neurovascular structures in this region: neurogenic (95%), venous (4%), and arterial (1%). Venous thoracic outlet syndrome (VTOS) will be the main topic of this review.
Anatomy
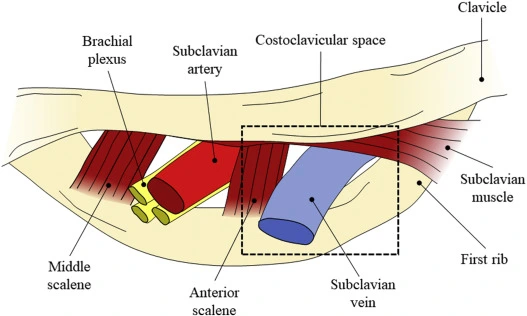
It is thought that recurrent abnormal and demanding interactions between the venous system and the thoracic outlet structures cause PSS. The anterior scalene muscle laterally, the costoclavicular ligament medially, the clavicle superiorly, and the first rib inferiorly all encircle the thoracic outlet. The axillary vein changes its name to the subclavian vein as it crosses the first rib and goes beneath the collarbone. The subclavian vein travels through the thoracic outlet to the internal jugular vein.
Venous endothelial cell injury, inflammation, scarring, and possible thrombosis result from long-term compression of the vein between the angle of the clavicle and the first rib during arm abduction. The costoclavicular ligament, which inserts more laterally in the majority of VTOS patients, contributes to subclavian vein compression. Furthermore, venous compression and damage may also result from the hypertrophy of nearby muscles, such as the anterior scalene and subclavius muscles.
Epidemiology
With a male-to-female ratio of 2:1, PSS is more frequently observed in younger individuals (in their 20s and 30s). These patients frequently don’t have any other serious health conditions. According to several studies, the incidence varies between 1 and 2 per 100,000 people annually. It happens on the right side more often. Venous TOS is more frequent than arterial TOS but less frequent than neurogenic TOS. PSS frequently affects athletes, particularly those who perform repetitive over-the-head arm motions, such as weightlifters, swimmers, rowers, and baseball or softball pitchers.
The three forms of VTOS are primary “Effort thrombosis,” secondary subclavian vein thrombosis, and intermittent blockage. Secondary thrombosis is not caused by compression and is typically caused by iatrogenic factors, such as the insertion of a pacemaker or catheter. Paget-Schroetter syndrome (PSS), often known as primary “effort thrombosis,” is linked to subclavian vein thrombosis and compression.
Causes of Paget-Schroetter syndrome
Thoracic outlet syndrome includes PSS. It occurs when a blood clot forms in one of the upper body’s deep veins. Younger persons without any other health problems are most likely to have it. Repetitive upward arm movements are one of the main causes.
PSS is sometimes referred to as “effort thrombosis” since it typically occurs with repeated upward arm motions, like those made when lifting weights, swimming, pitching, or the sports. However, it can also happen to people who don’t do these kinds of things. Another term for the production of blood clots is thrombosis.
The thrombosis is caused by compression of the region surrounding the subclavian vein and upward motions. Blood is returned to the heart via the subclavian vein from the upper body. The vein lining is harmed over time by this compression. Furthermore, the vein may have less space if there is muscular growth in that region. PSS is a kind of thoracic outlet syndrome, a collection of disorders in which a nerve or blood artery between the top rib and collarbone is compressed.
Among the risk factors for PSS are:
- Having no additional risk factors for blood clotting and being in your 20s or 30s.
- Having a cervical rib, often known as the “neck rib,” where the costoclavicular ligament, which joins the collarbone to the first rib, lateral insertion
An overdevelopment of the spine known as a “neck rib” is normally undetectable and does not result in any health issues. The term “lateral insertion” describes the position of the costoclavicular ligament in the body, which aids in shoulder joint stabilization. Males are twice as likely as girls to experience PSS, which usually occurs in the dominant arm’s shoulder.
Symptoms
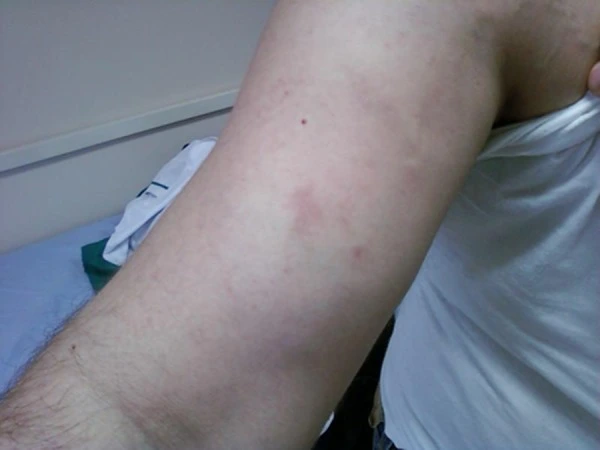
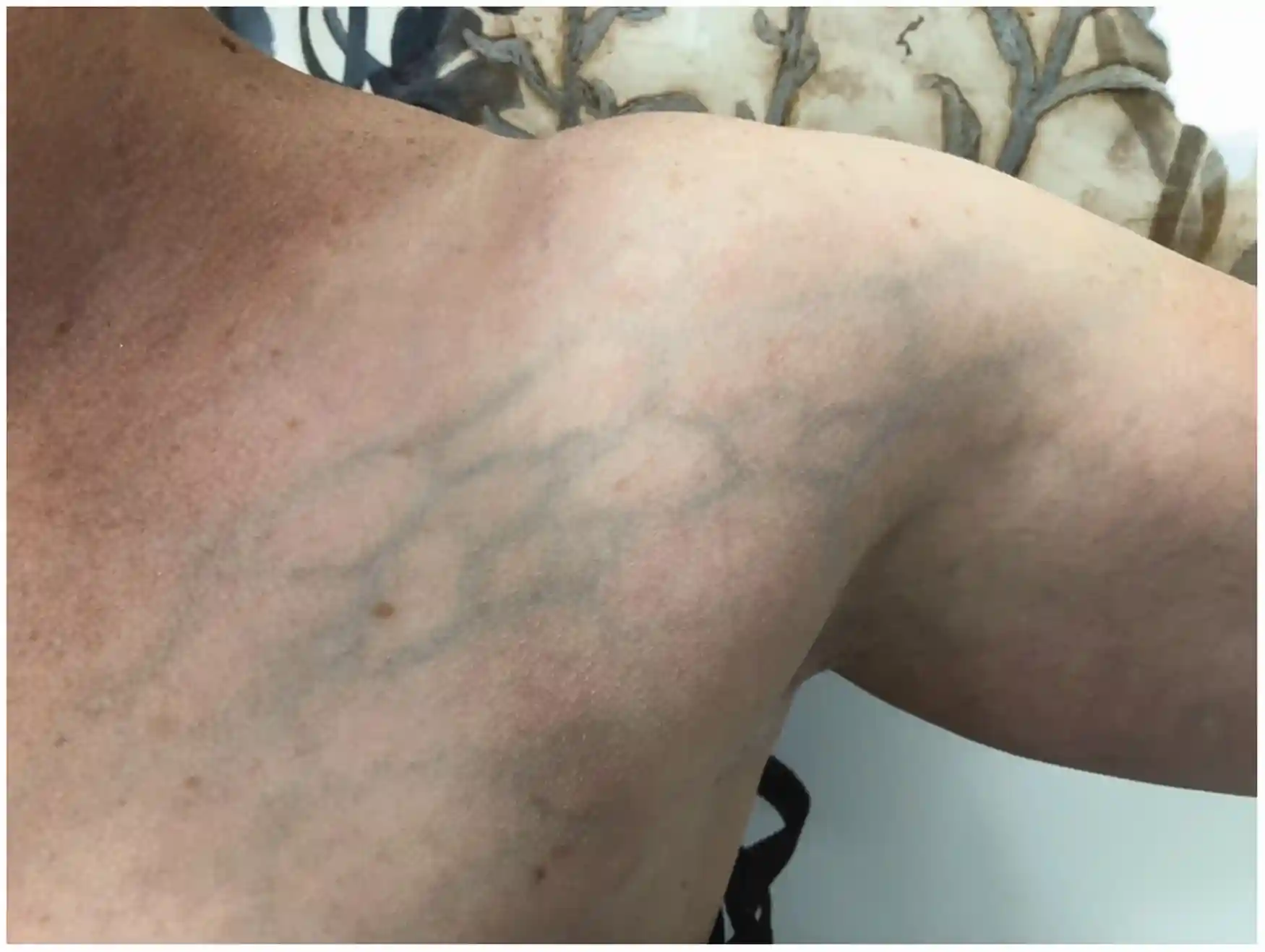
The most common presenting problems are arm pain and swelling. Heaviness, redness in the arms, cyanosis, and dilation, as well as visible veins on the upper arm and shoulder, are further symptoms. Acute or subacute symptoms typically appear first, though occasionally a patient may have chronic symptoms.
Occasionally, symptoms may be nonspecific or even like a strained muscle. The majority of patients report a specific triggering event, typically arm strain from sports. Occasionally, effort thrombosis can be triggered by small, relatively harmless daily tasks.
PSS can occasionally show no symptoms at all. However, it may have an impact on your arm’s appearance or how you feel.
PSS symptoms include:
- Pain in your arm, neck, or shoulder
- Swelling in your arm
- Changes in skin color on your arm
- Tenderness in your arm
- Veins you can see or feel.
Other symptoms of the illness include hand swelling or a dull aching in the shoulder.
Diagnosis
A history and physical examination are typically used to make the diagnosis, and imaging can be used to confirm it.
- Duplex ultrasonography, which is part of the first evaluation, shows partial or total thrombosis of the subclavian or axillary veins. According to reports, duplex imaging has 80–100% sensitivity and specificity, making it the gold standard for diagnosis.
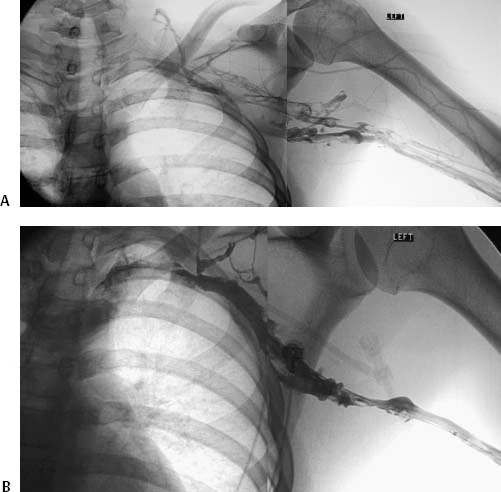
The diagnosis may be confirmed by additional imaging methods if duplex ultrasonography is not conclusive. Previously the gold standard for diagnostic imaging, catheter-directed venography is currently only used in situations with high clinical suspicion and equivocal non-invasive pictures because of its invasive nature, greater costs, and non-invasive ultrasound.
Computed tomographic (CT) or magnetic resonance imaging (MR) venography can also be used to examine the surrounding anatomy when atypical symptoms or equivocal ultrasonography are present. Both, though, have disadvantages. While MR is expensive and not widely available, CT venography is hampered by the possibility of contrast and radiation exposure.
The venography procedures listed above are available to clinicians who have a high clinical suspicion of upper extremity DVT and an inconclusive non-invasive ultrasound. If there is a high index of suspicion and no other explanation, suggest an algorithm to follow an equivocal Doppler ultrasound with MR venogram. In patients whose symptoms have been present for less than two to six weeks, catheter-directed thrombolysis and early thoracic outlet decompression are performed after a positive MR venogram.
Although there may be an increase in plasma D-dimer levels in upper extremity DVT, specificity varies between 14 and 60%. There are no recommendations for routine D-dimer testing because PSS is an uncommon condition. Although it is not advised as a confirmatory test, it can be helpful as an adjuvant therapy.
The guidelines for cancer screening after unexplained thromboses in the upper extremities are comparable to those for the lower extremities. Although routine screening is not advised, it can be taken into account in cases of inexplicable thromboses. A comprehensive history and physical examination, regular laboratory tests, abdominal ultrasonography, chest X-ray, and any other screenings tailored to a patient’s age or gender should be carried out in these situations.
Blood Tests
- Thrombophilia Panel: To screen for disorders that raise the risk of blood clots, such as mutations in certain genes (factor V Leiden, prothrombin gene) or deficiencies in specific proteins (protein C, protein S, antithrombin), a panel of blood tests may be ordered.
D-dimer Levels
- Although elevated D-dimer levels may be a sign of DVT, they are not a reliable indicator of Paget-Schroetter syndrome because they can also be elevated in other diseases.
Nerve Conduction Studies
- These tests may be carried out if the patient exhibits neuropathic symptoms, such as tingling or numbness.
Cancer Screening
- A comprehensive history and physical examination, regular laboratory tests, abdominal ultrasonography, chest X-ray, and other age or gender-specific screens should be carried out in cases of unexplained upper extremity thrombosis.
Treatment
There is no general agreement on the optimum course of action for managing effort thrombosis in the modern day. This uncertainty gets worse by the disease’s relative rarity, lack of awareness, and absence of extensive randomized trials. For long years, limb elevation and anticoagulation were the only conservative treatments for patients with effort thrombosis. However, further long-term statistics showed that this conservative approach had an unacceptably high frequency of recurrent thrombosis, disability, and persistent symptoms.
This has led to the development and assessment of aggressive treatment plans by clinicians that include:
- Venous bypass
- Thrombolysis
- Thrombectomy
- Percutaneous and surgical venoplasty
- Stents
Although systemic fibrinolysis is more effective than anticoagulation at maintaining vein patency, it is linked to increased risks of consequences, including cerebral hemorrhage. Local catheter-directed thrombolysis is currently advised for all patients who present early, since it has the therapeutic benefit of systemic thrombolysis without causing serious systemic side effects.
Since PSS is a deep vein thrombosis, the first line of treatment is to start anticoagulation medication, usually with an intravenous heparin drip. After receiving an initial intravenous heparin bolus, patients are maintained on an IV heparin drip. Both the maintenance heparin drip and the bolus dosage are weight-based. Levels or factor X levels are used to titrate the IV heparin drip. To lessen edema, the afflicted extremity should be raised.
It makes sense to think about a venogram and catheter-directed thrombolysis to lessen the clot stress if the patient shows up within two weeks of the onset of symptoms. A lysis catheter is inserted to drip a thrombolytic agent, like alteplase, for 24 to 48 hours under fluoroscopic guidance.
One should be aware of the possibility of acute kidney damage linked to hemolysis when utilizing pharmacochemical thrombectomy. Since the effectiveness of thrombolytic therapy is poor after that window of time, heparinization alone may be started without thrombolytic therapy if the presentation occurs more than two to four weeks after the onset of symptoms.
Mechanical catheter-directed thrombectomy is an additional therapeutic alternative. Early in the disease’s progression, this must be done. Surgery may also be suggested by a physician to alleviate vein constriction. What’s applying pressure to the area will determine the kind of operation you require. However, choices include:
- Removing the rib entirely or in part
- Breaking up the scar tissue surrounding the vein, removing a portion of the costoclavicular ligament, and removing a portion of the surrounding muscle
- Stents can be inserted into the vein to maintain its opening, although surgery is a more long-term solution for PSS.
Prognosis
Up to 90% of patients may benefit from a combination of thrombolysis and thoracic outlet decompression. Though less effective than thrombolysis and decompression, anticoagulation plus decompression still produces better outcomes than anticoagulation alone.
Complications
- Pulmonary embolism
- Post-thrombotic syndrome
- Recurrent thrombosis
Conclusion
- Thoracic outlet syndrome includes PSS. It occurs when a blood clot forms in one of the upper body’s deep veins.
- Younger persons without any other health conditions are most likely to have it. Repetitive upward arm movements are one of the main causes.
- Blood-thinning drugs, thrombolysis to remove the clot, and decompression surgery to release venous pressure are all part of the treatment.
FAQs
Paget-Schroetter syndrome effort thrombosis: what is it?
Young, active persons who participate in sports or whose jobs include repetitive arm motions are most frequently affected by effort thrombosis, also known as Paget-Schroetter syndrome. This condition causes trauma to the axillary-subclavian vein, which in turn triggers deep vein thrombosis.
What other terms are used to describe Paget-Schroetter syndrome?
This syndrome is also known as “spontaneous” thrombosis of the upper extremities, Paget-Schroetter syndrome, venous thoracic outlet syndrome, or exertion thrombosis. It can be brought on by congenital characteristics, including excess muscle, cervical ribs, or anomalies in tendon insertion.
How is effort thrombosis treated?
Rather, routine catheter-directed thrombolysis, early TOD in suitable individuals, and physical and occupational rehabilitation are the best ways to control effort thrombosis. Patients with coexisting thrombophilia and poor surgical outcomes may benefit from long-term anticoagulation.
What is the Paget-Schroetter treatment?
Although rib excision is the final treatment, venoplasty and stenting without decompression may yield positive results. The surgical technique may be supraclavicular, infra-clavicular, or trans axillary. There is much disagreement over when decompression should occur following thrombolytic treatment.
Which age range is affected by Paget-Schroetter syndrome?
Roughly 80% of Paget-Schroetter syndrome patients report engaging in physically demanding activities that require their upper extremities. One with a 2:1 male-to-female ratio, the syndrome is more prevalent in men, and the typical age of these individuals upon presentation is in their early 30s.
How should thrombosis be treated right away?
Blood thinning drugs (anticoagulation), such as heparin and warfarin (Coumadin), are the standard of care for treating acute DVT. Blood thinning drugs function by letting blood circulate a trapped clot while blocking the clot’s passage to the lungs.
What is the Paget’s disease diet?
Patients with Paget’s disease of the bone do not require a special diet, but those on bisphosphonates should make sure they are getting enough calcium and vitamin D. Given the significant risk of fractures, vigorous physical activity is not advised. Low-intensity muscle-strengthening exercise is advised, nevertheless.
Reference
- Saleem, T., & Baril, D. T. (2023, April 26). Paget-Schroetter Syndrome. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK482416/
- Schwenke, M., Goldman, R. E., Sarkeshik, A. A., & King, E. C. (2022). Subclavian Effort Thrombosis: Pathophysiology, Diagnosis, and Management. Seminars in Interventional Radiology, 39(03), 304–311. https://doi.org/10.1055/s-0042-1753481
- Paget–Schroetter Wikipedia contributors. (2024a, August 26). Paget–Schroetter disease. Wikipedia. https://en.wikipedia.org/wiki/Paget%E2%80%93Schroetter_disease
- Lovering, C. (2024, September 6). What is Paget-Schroetter Syndrome? Healthline. https://www.healthline.com/health/paget-schroetter-syndrome#outlook
- Gaillard, F., & D’Souza, D. (2008). Paget-Schrötter syndrome. Radiopaedia.org. https://doi.org/10.53347/rid-1825